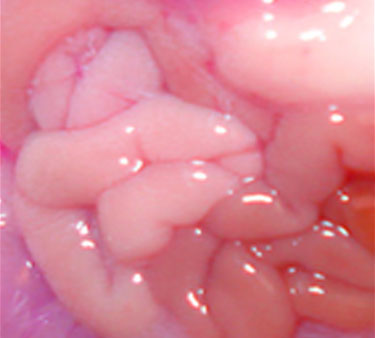
Development
As the aetiology and pathogenesis of NEC are not yet completely understood, accurate models are crucial in deciphering the complexity of the disease and discussion of various models was a key element of the 2016 SIGNEC conference.
In his presentation, Piglet model for spontaneous NEC mechanisms and clinically relevant interventions, Prof Per Sangild of the University of Copenhagen explained the rationale behind research in preterm piglets, which share greater similarity to human NEC than rodents and are easier to deliver preterm. Piglets are also helping us to understand the long- term consequences of NEC and prematurity.
In The trifecta for a severe mouse model of NEC: Formula feeds, hypoxia and NECteria, Misty Good, Assistant Professor of Pediatrics at the Children’s Hospital of Pittsburgh, talked about how mouse NEC models provide the ability of genetic manipulation to study the pathogenesis of the disease. She said it is imperative that modelling evolves to more readily count for nuances as further understanding of the disease develops.
Modelling now includes valuable insights provided by rhesus macaque monkeys. Professor David Hackam of Johns Hopkins Hospital told the conference that NEC is a naturally occurring disease in these monkeys and dramatically like human NEC. Their intestinal immune system is, he said, very similar to humans.
Dr Good decided to dedicate her career to studying NEC whilst working in The Hackam Lab , which is dedicated to understanding the cellular and molecular events leading to NEC. Her presentations included this slide, which depicts their hypothesis of how NEC happens:

Gram negative bacteria are present in the lumen of the intestine and express LPS (Lipopolysaccharide). LPS activates the innate immune receptor Toll-like receptor 4 (TLR4) and under stressful conditions such as prematurity, formula feeding and exposure to hypoxia leads to enterocyte and intestinal stem cell apoptosis, impaired intestinal restitution, and reduced enterocyte proliferation. This allows bacterial translocation leading to an exaggerated inflammatory response, all of which are hallmarks of NEC.
In The Role of MicroRNAs in NEC, Dr Good spoke of recent interest in these small, functional noncoding RNAs which have been implicated in intestinal inflammation and barrier function. As miRNAs are known to be differentially expressed in intestinal inflammatory states, The Good Lab hypothesized that miRNAs are differentially expressed in premature infants with NEC. Data confirmed this and that miR-17 and the miR-17~92 cluster may be important in the pathogenesis of NEC.
At SIGNEC 2015, Dr Steven McElroy of the University of Iowa posed the question Is the Paneth cell the missing link to NEC? and in 2016 he spoke further on Paneth cells and their potential role in the development of NEC. These granulated cells at the base of the intestinal glands play several roles within the intestine and babies who develop NEC have significantly fewer Paneth cells. The Steven McElroy Laboratory has developed a new animal model of NEC that is dependent on the disruption of Paneth cells followed by enteral gavage of Klebsiella pneumoniae. It has consistently and significantly resulted in intestinal injury with the key hallmarks seen in infants with NEC, and Paneth cells may alter LPS levels and TLR4 activation.
This and similar work has led researchers to ask the question whether NEC may be several diseases that come together in a final common pathway.
NEC is certainly over-complex, which is how Professor Boris Kramer of Maastricht University Medical Center in the Netherlands described the subject of his 2016 presentation The development of NEC and the gut-brain axis – more than gut feelings! Innervation of the gut plus metabolites from the microbiome drive voiding, and low frequency of voiding of the gut may precede NEC.
While the role of bacterial infection in the pathogenesis of NEC has been studied intensively, in Blood transfusion and intestinal perfusion in preterm infants, Dr Narendra Aladangady of Homerton University Hospital in London pointed out that little investigation of the impact of anaemia and blood transfusion on organ perfusion has taken place even though the majority of VLBW infants receive transfusions.
Related Research
1. Necrotizing enterocolitis: new insights into pathogenesis and mechanisms
Authors: Diego F. Niño, Chhinder P. Sodhi, and David J. Hackam
doi:10.1038/nrgastro.2016.119
Published August 2016
2. Increased Intestinal Inflammation and Digestive Dysfunction in Preterm Pigs with Severe Necrotizing Enterocolitis
Authors: Støy, Ann Cathrine F; Heegaard, Peter M. H.; Skovgaard, Kerstin; Bering, Stine B.; Bjerre, Mette; Sangild, Per T.
Neonatology, Vol. 111, 2017, s. 289-296
Published May 2017
3. Animal models of gastrointestinal and liver diseases. Animal models of necrotizing enterocolitis: pathophysiology, translational relevance, and challenges.
Authors:Lu P, Sodhi CP, Jia H, Shaffiey S, Good M, Branca MF, Hackam DJ
Am J Physiol Gastrointest Liver Physiol. 2014 Jun 1; 306(11):G917-28.
doi: 10.1152/ajpgi.00422.2013.
Published April 2014
4. Paneth-cell-disruption-induced necrotizing enterocolitis in mice requires live bacteria and occurs independently of TLR4 signaling
Authors: White JR, Gong H, Pope B, Schlievert P, McElroy SJ
Dis Model Mech. 2017 Jun 1;10(6):727-736. doi: 10.1242/dmm.028589
Published April 2017
5. Blood transfusion in preterm infants improves intestinal tissue oxygenation without alteration in blood flow.
Authors: Banerjee, Jayanta & Leung, Terence & Aladangady, Narendra.
Vox Sanguinis. 111. . 10.1111/vox.12436.
Published August 2016
Warning
This section is intended for professionals with an interest in necrotizing enterocolitis. It is not intended for the families of babies who are currently receiving care in a neonatal unit or who previously had a baby cared for in a neonatal unit. It contains information and images which they may find distressing. They should visit our For Families section.